People with depression crave carbs more and find less reward in fats & proteins.
Could the gut-brain axis explain this? 🧵1/14
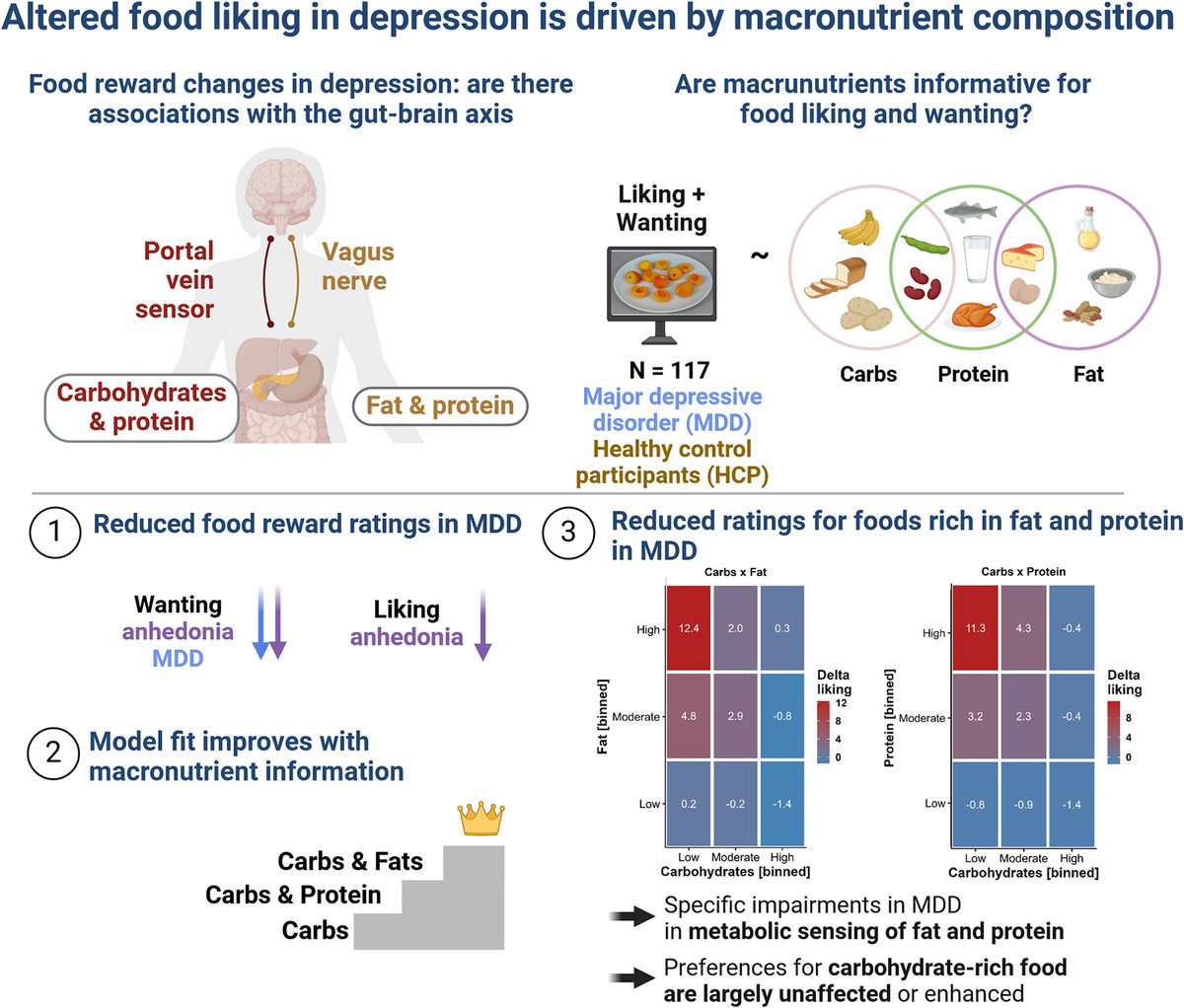
Each person completed a food cue reactivity task, where they rated how much they liked and wanted different foods. /2

🧠 They had lower "wanting" scores but similar "liking" scores.
🥖 They showed a stronger preference for carbohydrate-rich foods.
🥑 They had lower preference for high-fat & high-protein foods.
Carbs seemed to compensate for the lower reward they experienced with fats & proteins. /3

❌ Wanted and liked fat-rich foods less
❌ Wanted and liked protein-rich foods less
✅ Preferred carbohydrate-rich foods more /4

The study suggests that depression disrupts the gut-brain axis, which plays a key role in food reward.
People with MDD may have impaired fat and protein reward signaling while their response to carbohydrates remains intact. /5

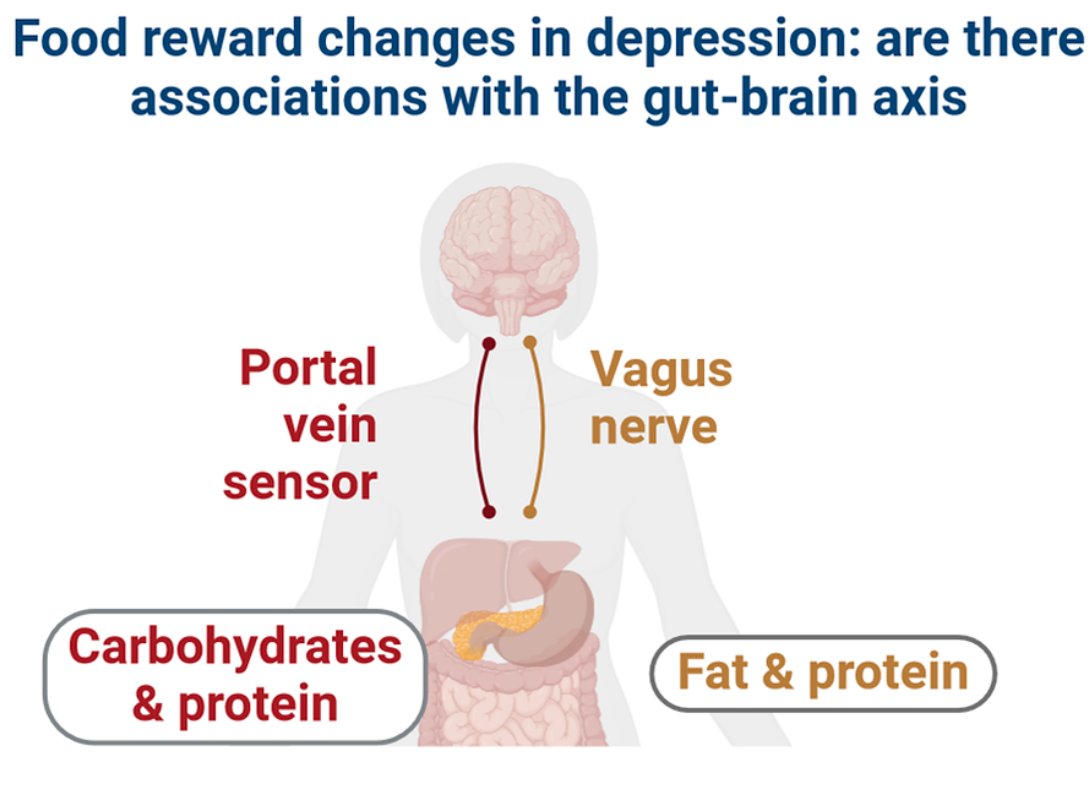
🔹 Fat signaling relies on vagus nerve pathways.
🔹 Carbohydrate signaling uses spinal and portal vein sensors.
🔹 Protein signaling is more complex.
MDD may impair fat/protein reward signaling, but not carbs. /6
Interestingly, insulin resistance (HOMA-IR) and ghrelin levels were not strongly linked to these food reward changes.
However, people with MDD had higher insulin resistance, which could still play a role in how appetite is regulated. /7
The study was cross-sectional, meaning it can’t prove cause and effect. It didn’t measure whether people perceived foods as unhealthy. It didn’t differentiate between fat types (e.g., saturated vs. unsaturated). Despite this, the study offers new insights into how depression alters food reward processing. /8
It’s unclear whether depression drives carb cravings or if a biological preference for carbs contributes to depression. The relationship is likely bidirectional, making future research critical. /9
✅ Carbohydrate cravings may play a role in mood regulation.
✅ Future studies should explore gut-brain interventions to address depression-related appetite changes. /10
🔹 Gut-brain signaling disruptions may play a major role in this imbalance.
🔹 Mood and anxiety symptoms seem to influence macronutrient preferences more than metabolic factors.
This could help explain why many people with depression report increased cravings for processed, carbohydrate-heavy foods. /11
Could dietary changes that restore fat and protein perception improve mood symptoms?
Could vagus nerve stimulation help normalize food reward responses?
How do different types of carbs, fats, and proteins affect mood and appetite regulation? /12

More from this author
High altitude climbing may cause irreversible brain damage 🧵1/11 https://t.co/jV9CvhzHvC
As Resident Doctors, we work 26h shifts with no sleep. Coffee wasn’t enough to keep me sharp, so I dove into the literature for other solutions. Her...
Magnesium-L-Threonate (1g/day) vs. Placebo for Sleep Difficulties: 🛌 Improved deep & REM sleep ⚡ Increased energy & daytime productivity 🧠 Bet...
⏳ Your chronotype—night owl or morning lark—determines when you perform at your best. Here's how to align tasks with your body’s clock helps you work...
Recent Threads
taekook taguan ng anak au wherein jk received a surprising gift from their xmas party… [ christmas special 🎄] https://t.co/WY3C450KpV
@HitWithAHeart I hear him before I see him. The weight of his steps on the stairs. Slower than usual. Measured. Like he’s already bracing for whatev...
(1/7) I'm not going to do a full trailer breakdown for Zach Cregger's Resident Evil film, since we have an early form of the script you can place a lo...
Nikola Jokic is 0-6 against 50+ win teams in the playoffs. https://t.co/l5hCeVCoUj
Uni is a fighter! https://t.co/AXkBVFJ2My
Triggered girl at comedy show… https://t.co/z1BC2qG7Rd
Popular Threads
Top 20 Players with the most goals + assists in football history, only players with assists available (following the Opta criteria for assists) Seaso...
Please retweet and share if you support my and others' vaccine injury recoveries. https://t.co/y8xNWwRUOO
The ICT Mentorship Core Content Month 1 Summarized: https://t.co/6tXJxPMDhm
ICT’s 2022 Mentorship Summarized: https://t.co/zFJCgIfDAR
A thread: Pakistani newspaper Dawn's front pages from 4th december 1971 to 20 December to see how they kept their own people in the dark. This was on...
DON'T ARGUE WITH DONKEYS (Fable) The donkey said to the tiger: - "The grass is blue". The tiger replied: - "No, the grass is green." The discussion...













